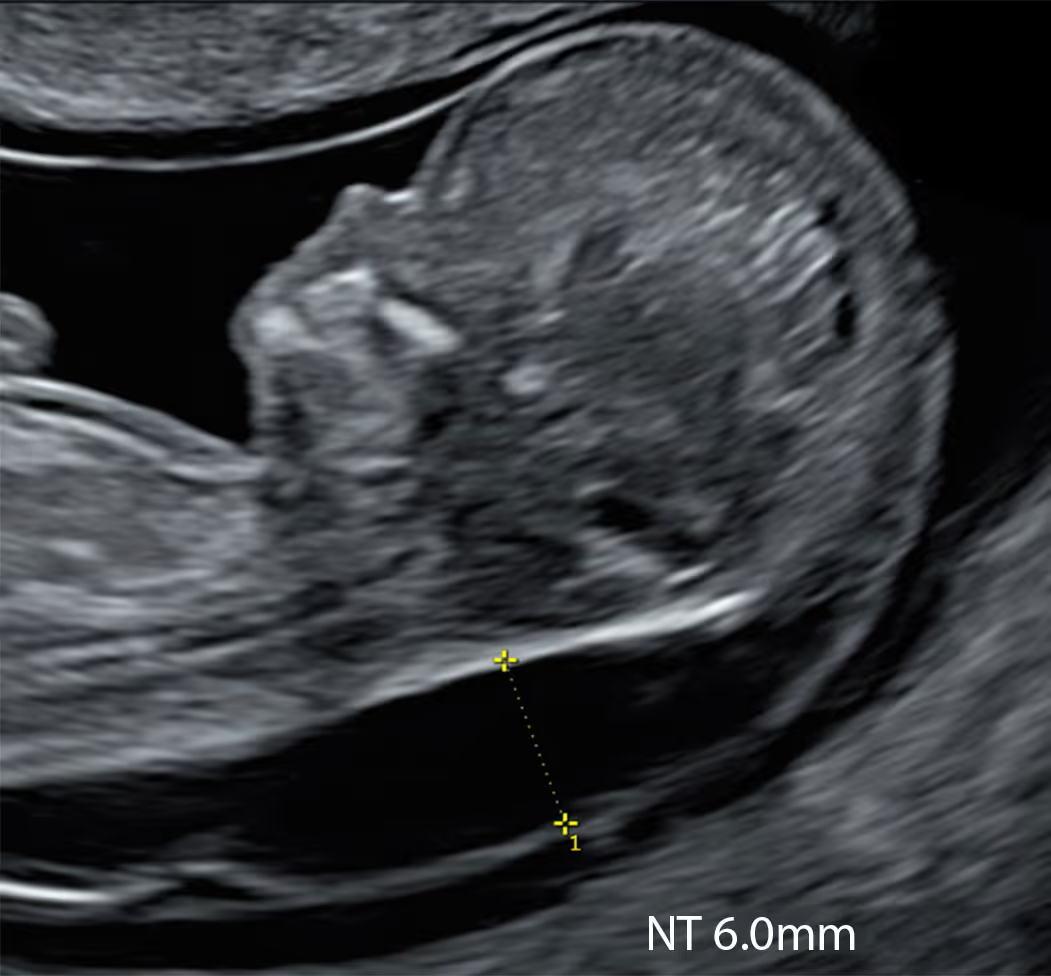
SMART NT Step One:
Combining the earliest structural screening for most severe anomalies with precise NT measurement in a single scan
At 10 weeks, the fetus is usually about 30–40 mm (CRL), roughly the size of a strawberry or a small apricot.
At 10 weeks, an NT measurement of ≥2.5 mm is considered abnormal and, is associated with an ~40% chance of an adverse pregnancy outcome.
Acrania, alobar holoprosencephaly, spina bifida, absence of arms/legs, encephalocele, omphalocele with liver, amniotic band syndrome, body stalk anomaly, sirenomelia, cloacal exstrophy.
In normal pregnancies, fetal heart rate (FHR) peaks around 9–10 weeks at about ~170 bpm (often roughly 160–180 bpm)
One-stop 10 Week Scan + NIPT. If iNT (NT ≥2.5 mm; CRL <45mm) is found, we recommend proceeding with KNOVA. If NT is normal, KNOVA is optional; we advise to discuss basic versus advanced NIPT and choose according to context and preference.
Apart from measuring NT, the 10-week scan can reveal lethal non-genetic anomalies and features suggestive of a genetic condition. Lethal non-genetic anomalies are NIPT exclusion criteria; when findings suggest a genetic cause, KNOVA is the preferred screen.
According to recent data, an NT measurement of 2.5 mm or greater at 10 weeks is associated with an abnormal fetal outcome in about 42% of cases. This cut-off has been adopted in our protocol, and any measurement at or above this level triggers the SMART NT pathway. It is important to note that this value is higher than the 95th centile for this stage of pregnancy, which is typically 2.1–2.4 mm.
Learn More about the SMART Protocol

Alobar holoprosencephaly, heart defects, limb abnormalities, exomphalos with liver, and particularly early fetal hydrops or cystic hygroma are strongly associated with chromosomal or genetic syndromes. At later stages, these findings usually warrant diagnostic testing (CVS); however, CVS cannot be performed safely at 10 weeks. In such cases, we recommend starting with a genomic NIPT as the first step. A high-chance NIPT result, especially for monogenic conditions, can help guide the planning of further diagnostic tests.

Learn More about the SMART Protocol

Acrania, body stalk anomaly, cloacal exstrophy, pentalogy of Cantrell, sirenomelia, amniotic band syndrome, and limb–body–wall complex are usually NOT associated with genetic conditions. Most of these anomalies are lethal or have an extremely poor outcome. If such conditions are detected at 10 weeks, we strongly recommend NOT proceeding with NIPT, as performing it may delay appropriate referral and management, and a low-risk result could provide false reassurance.

Learn More about the SMART Protocol

The SMART NT protocol cannot be used in certain situations where genomic NIPT (KNOVA) is not applicable. These include early not genetic fetal anomalies, twin or triplet pregnancies, vanishing twin, donor egg IVF pregnancies. Maternal ineligibility includes cases where the mother has a history of recent cancer, organ or bone marrow transplantation. In such cases, the fetal cfDNA in the mother’s blood cannot be accurately analysed, making genomic NIPT unreliable.
Genetic testing looks at your DNA to find changes or variants in your genes. These changes can tell us if you’re at risk for certain inherited conditions, like hereditary cancers or if you’re a carrier for a genetic condition.
It can reveal if you have a higher genetic risk for certain cancers (like breast, ovarian or bowel), if you’re a carrier for inherited conditions, or if you have a genetic condition that could impact your health or your family’s.
No — genetic testing shows your risk, not a guarantee. Some people with a genetic variant never develop the condition, while others without a variant might still be affected due to lifestyle or environmental factors.
No — genetic testing shows your risk, not a guarantee. Some people with a genetic variant never develop the condition, while others without a variant might still be affected due to lifestyle or environmental factors.
The best approach is to use both — starting with a transabdominal scan (TAS) and then offering a transvaginal scan (TVS) for a more detailed assessment.
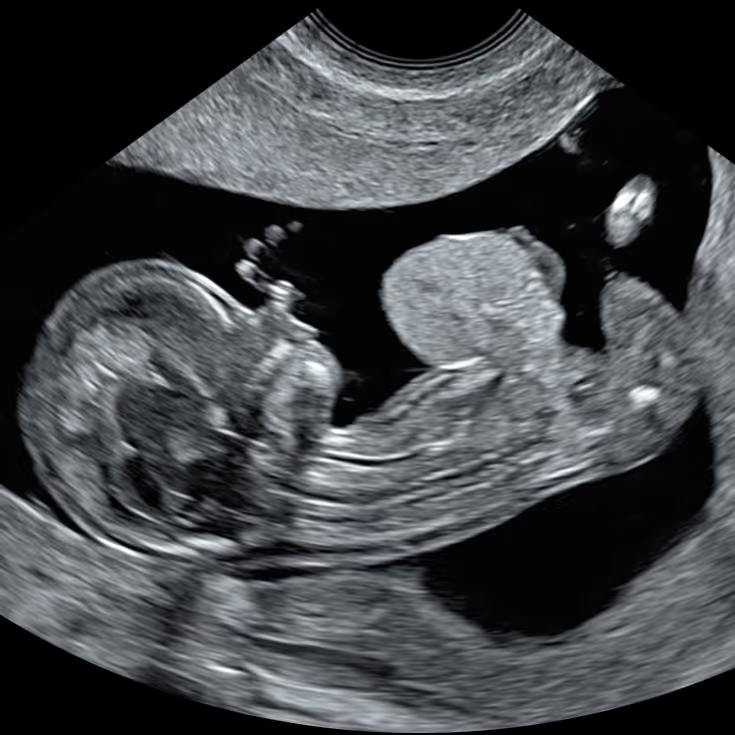
We begin with TAS. No full bladder is needed, and in most cases TAS provides excellent diagnostic images to confirm the number of babies, document the heartbeat, observe fetal movements, and measure the crown–rump length (CRL). In many pregnancies, TAS is also preferred for measuring the NT at 10 weeks because, due to gravity, the baby often lies on its back, which can make the mid-sagittal view easier to obtain.
TAS can give a useful overview of early fetal anatomy, but a precise, structured assessment of fetal structures at 10 weeks is usually better with TVS. Once we have obtained as much information as possible abdominally, we offer TVS. In our experience, most patients choose to proceed, as TVS typically provides the highest-resolution views for early anatomy and can also help with NT measurement when the fetal position is optimal.
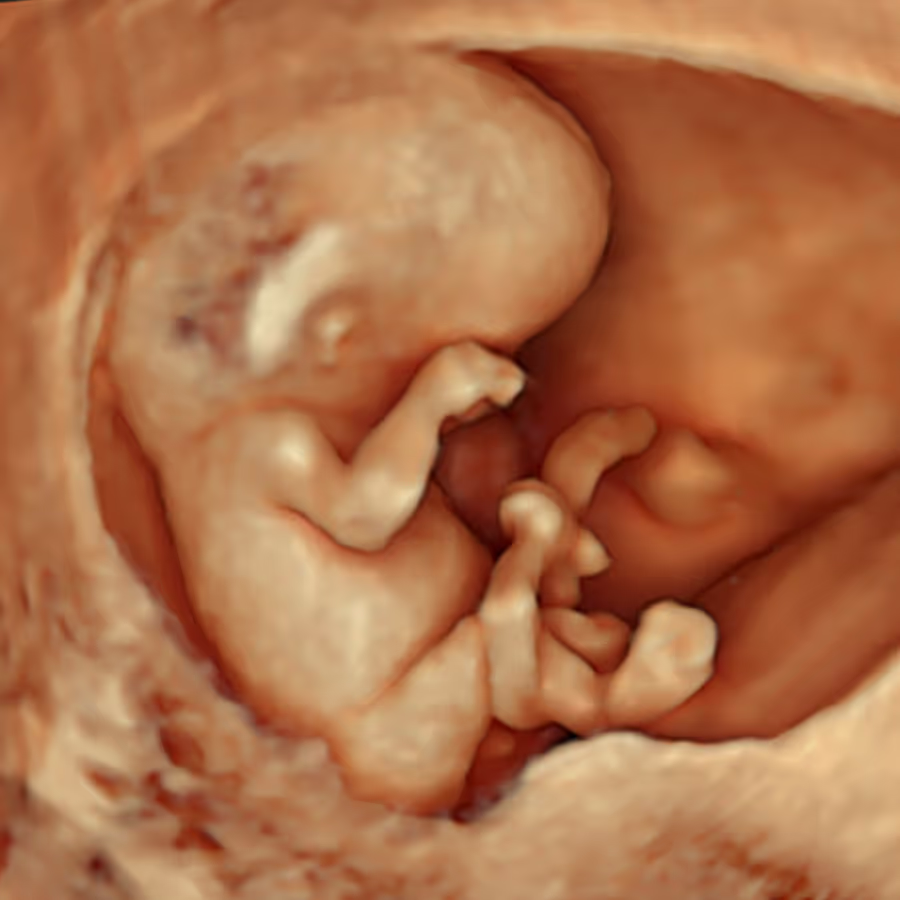
If the baby’s position is not suitable for a direct NT measurement (for example, an oblique or coronal view), there is also the option of using a reconstructed 3D dataset to obtain an accurate measurement.
It’s simple — you speak with one of our expert Genetic Counsellors, receive a home kit in the post, collect a cheek swab, and send it back. Your DNA is analysed in a UK or US lab, and results are ready in under 4 weeks.
Yes. At Jeen Health, your data is encrypted and stored securely on our GDPR compliant servers, as well as with our vetted laboratories. Your results are only shared with you and your dedicated Genetic Counsellor, never with insurers or third parties.
Not at all. While a strong family history increases your risk, many people with genetic conditions have no known family history. Testing helps you uncover hidden risks you wouldn’t otherwise know about.
Not at all. While a strong family history increases your risk, many people with genetic conditions have no known family history. Testing helps you uncover hidden risks you wouldn’t otherwise know about.
NT scan and NIPT at 10 weeks, then full results by week 12
1
If increased NT is found, you can have the SMART Test straight away
2
Receive genetic results in 2 weeks
3
Top-to-toe expert fetal examination
Disclaimer! These reflections are my own and arise from practice rather than committee. They do not represent the positions of the FMF, UCLH, NHS, RCOG, ISUOG, or any other organisation. As with any clinician, I may make mistakes or misjudgements. In my view, a carefully performed 10 Week Scan, used alongside appropriately selected modern NIPT and followed by targeted diagnostic testing when indicated, can provide a balanced clinical approach by supporting earlier risk assessment while avoiding unnecessary intervention or over-interpretation. Dr Fred Ushakov
For medical professionals who want to learn more about the SMART NT approach, access training, and join our clinical network.