The period between 11 and 14 weeks, when the fetal crown–rump length (CRL) measures 45–84 mm, is the standard time for NT measurement
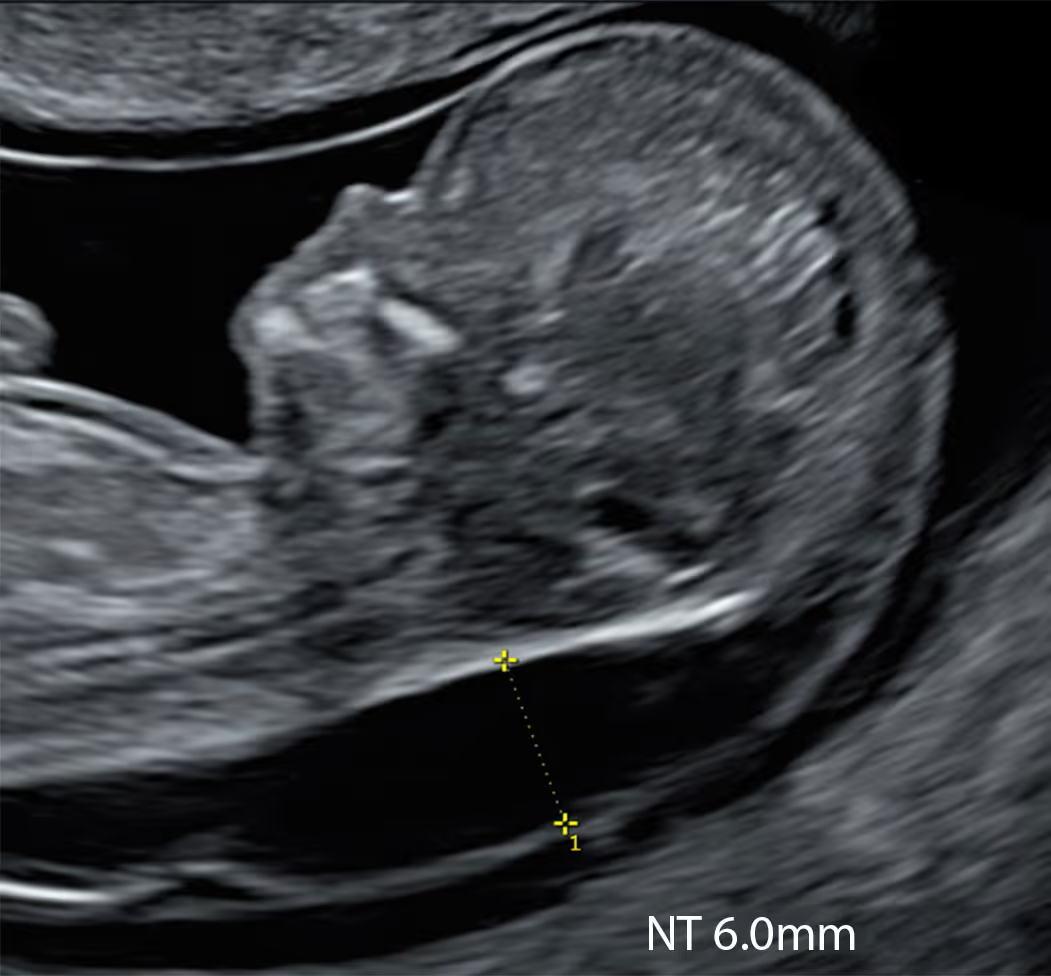
The nuchal translucency (NT) normally disappears after 14 weeks of pregnancy. From around 15 to 20 weeks, the same region is assessed using a different ultrasound marker called the nuchal fold (NF) measurement, which becomes the standard marker for detecting chromosomal abnormalities during the second trimester.
An NF thickness of 6.0 mm or more is considered abnormal. This cut-off has been validated only for the period between 15 and 20 weeks of gestation. After 20 weeks, the nuchal fold naturally thickens as part of normal growth; therefore, the 6 mm threshold should be interpreted with caution.
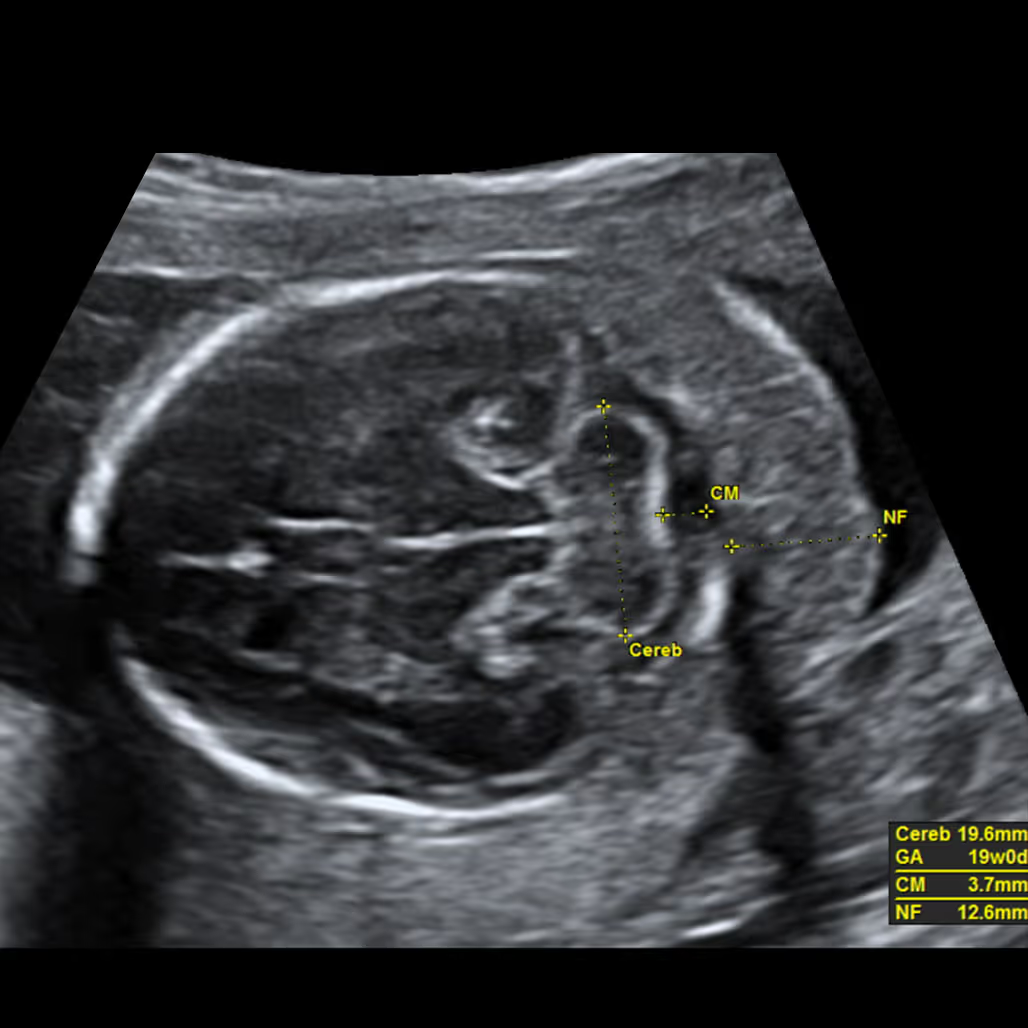
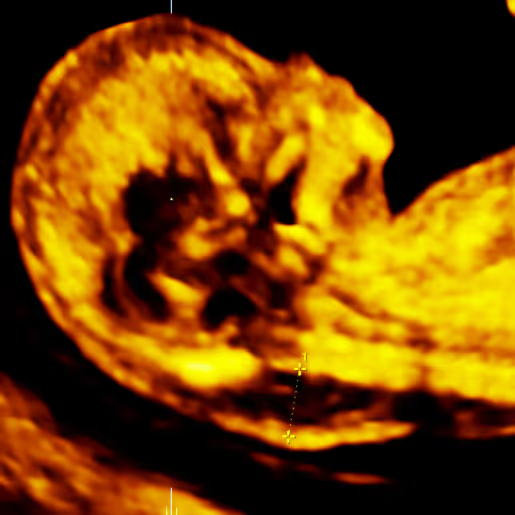
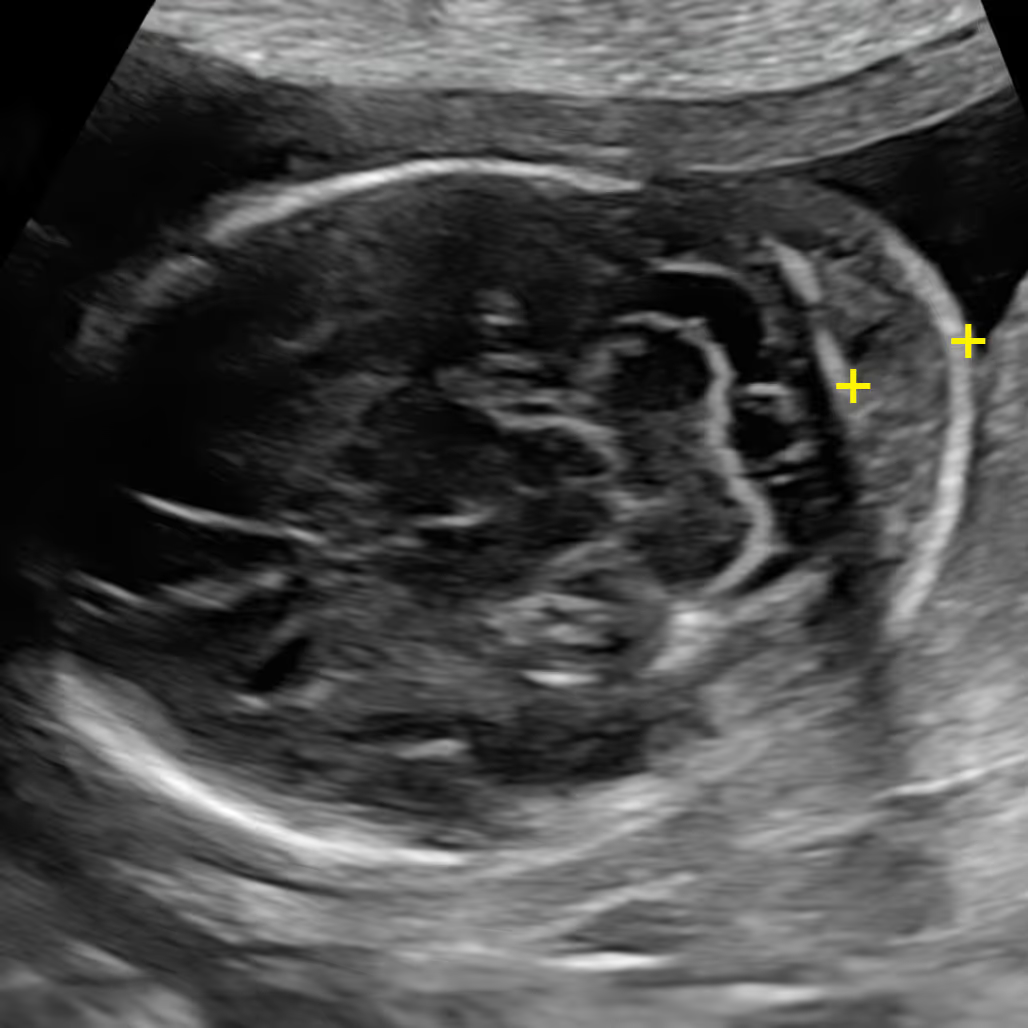
The nuchal fold (NF) is the thickness of the soft tissue (not fluid) at the back of the fetal neck. Increased NF is an ultrasound feature, not an anomaly. It was originally described by Prof Beryl Benacerraf in 1985 in the United States as the first soft marker for Down syndrome. The correct measurement of the nuchal fold in the second-trimester fetus is performed at the level of the posterior fossa, on a modified transverse view of the fetal head that includes the thalami, cerebellar hemispheres, and occipital bone. The NF is measured by placing the electronic callipers from the outer edge of the occipital bone to the outer skin surface.
Learn More about the SMART Protocol

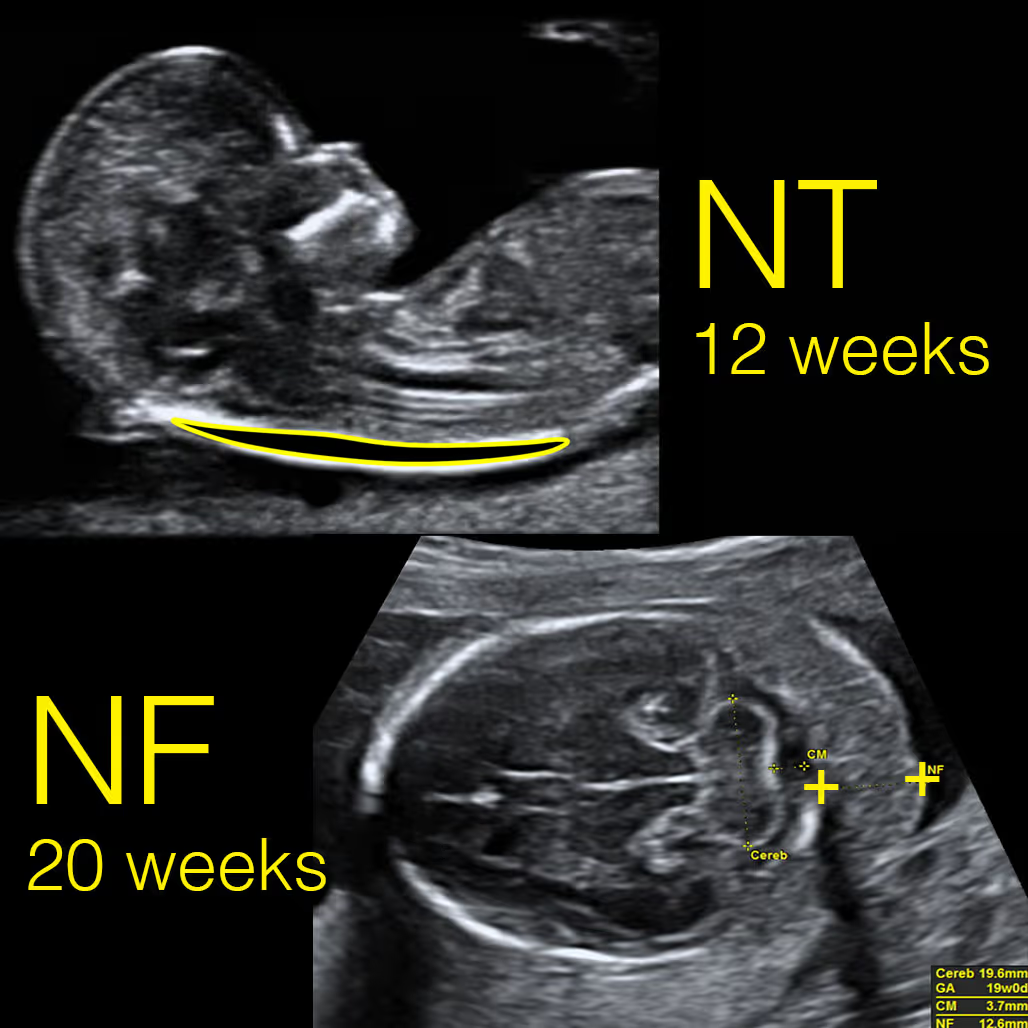
Both NT and NF look at the area at the back of the baby’s neck, but at different stages of pregnancy. NT (nuchal translucency) is a small pocket of fluid seen on the 11–14 week scan. It usually disappears after 14 weeks. NF (nuchal fold) is measured later, around 15–20 weeks, and looks at the soft tissue thickness instead of fluid. A thick NF can sometimes be a sign of certain chromosome conditions such as Down syndrome.
Learn More about the SMART Protocol

No. Although in some cases a persistently high NT may evolve into nuchal fold thickening later in pregnancy, in most cases a thickened NF develops independently, even in babies that previously had a normal NT. This means that the NF is a separate ultrasound marker, usually appearing on its own and at a later stage.
Learn More about the SMART Protocol

Trisomy 21 (Down syndrome), trisomy 18 (Edwards syndrome), trisomy 13 (Patau syndrome), monosomy x (Turner syndrome), triploidy, Noonan syndrome, Costello syndrome, other rasopathies, congenital heart defects, fetal hydrops, lymphatic disorders, skeletal dysplasias, Kabuki syndrome, intrauterine infection.
There are three different periods when nuchal thickness can be measured
At 10 weeks, NT can be measured accurately and may be a more sensitive early sign of possible problems, allowing prompt reassurance or testing.
This is the traditional time for NT assessment as part of the Combined Screening Test (CST). In the UK and many other countries, most babies have their NT measured during this stage of pregnancy.
After 14 weeks, the fluid behind the baby’s neck usually disappears, making the NT measurement unreliable. Instead, a different marker called the nuchal fold (NF) can be measured at this stage.
The nuchal fold is a small skin fold at the back of your baby’s neck that can sometimes look a bit thicker if certain conditions (especially trisomy 21) are present.
It is usually measured at the detailed 18–21-week scan as one of several “soft markers” that can give extra information about your baby’s health.
In most pregnancies between 15 and 20 weeks, a nuchal fold measuring less than 6.0 mm is considered normal.
If your baby’s nuchal fold is 6.0 mm or more, your report will usually describe it as “increased” or “thickened”. On its own it is a soft marker, not a diagnosis, and many babies with a thick nuchal fold are born completely healthy.
If you already had a low-chance NIPT result, this is very reassuring because NIPT has a very high negative predictive value for Down syndrome (T21). In this situation, an isolated thick nuchal fold usually adds only a small extra concern.
You should still be offered a detailed expert scan of your baby by a fetal medicine specialist (in an FMU or a specialist private clinic). You may also be offered the option of an amniocentesis. This is a diagnostic test that looks directly at the baby’s chromosomes, but it is invasive and carries a small risk of miscarriage, so the pros and cons should be carefully discussed with you by a fetal medicine doctor.
You should be offered a detailed expert scan in a Fetal Medicine Unit (FMU) or with a private fetal medicine specialist to check the baby thoroughly, especially the heart and face. Depending on your previous screening, you may also be offered NIPT (if not already done) or diagnostic testing such as amniocentesis.
Usually, a follow-up scan is recommended to make sure the baby continues to look well and to exclude the small possibility of developing generalised skin swelling (oedema) or hydrops.
Not usually. Unlike an increased nuchal translucency (NT) in early pregnancy, which is clearly associated with congenital heart disease, the link between an increased nuchal fold and heart problems in babies without a chromosomal condition is less well documented and probably weaker.
However, a thick nuchal fold can sometimes be seen in babies with heart defects. For this reason, your baby’s heart should be examined very carefully by an expert – either as part of a detailed fetal medicine scan or in a separate specialist heart scan (fetal echocardiogram), depending on the pathway with your antenatal care provider.
Yes. In some babies, the nuchal fold in the second trimester remains thick after an increased nuchal translucency (NT) was seen in the first trimester, and this combination is generally a less favourable sign.
If you have already had an invasive test (CVS or amniocentesis) and the results of rapid aneuploidy testing (QF-PCR) and chromosomal microarray (CMA) are normal, a persistently increased nuchal fold can raise the possibility of an underlying single-gene (monogenic) or other non-chromosomal condition, such as a RASopathy (for example, Noonan syndrome).
In this situation, more detailed genetic testing – such as exome sequencing or whole-genome sequencing (WGS) – may be very helpful, and referral to fetal medicine and clinical genetics for specialist counselling is usually recommended.
If you miss this window, you can no longer have the NT-based combined test, but you may be offered a later second-trimester blood test (the “quadruple test”), and you will still be offered the detailed 20-week anomaly scan with NF measurement.
It is important to understand that the quadruple test has limited value, and a significant proportion of babies with Down syndrome will not be identified by this screening. The second-trimester scan is very useful for detecting structural anomalies, particularly those associated with Edwards and Patau syndromes; however, it is relatively insensitive for Down syndrome on its own.
For this reason, many professionals will recommend proceeding with NIPT, which continues to work very well even at later gestations.
Yes. The measurement of NF is technically quite challenging and can change if the baby’s head and neck are extended or flexed, or if the baby is moving. This is why it should be done by an experienced sonographer or fetal medicine specialist, and sometimes repeated if the position is not ideal.
No. Nuchal translucency (NT) is a fluid space measured at the back of the neck in the first trimester (around 11–13 weeks).
The nuchal fold (NF) is a different measurement of the skin and underlying tissue at the back of the neck in the second trimester (around 18–21 weeks).
Not at all. While a strong family history increases your risk, many people with genetic conditions have no known family history. Testing helps you uncover hidden risks you wouldn’t otherwise know about.
The nuchal fold is usually measured once and not routinely followed through the rest of the pregnancy. This is because this part of the baby’s neck naturally becomes thicker as the baby grows, so later measurements are harder to interpret. There are no good studies on nuchal fold measurements after 20 weeks, and the commonly used 6.0 mm cut-off has not been clearly validated beyond this stage.
However, some fetal medicine specialists may suggest a follow-up scan to make sure the baby continues to look well and to exclude the very small possibility of generalised skin swelling (oedema) or hydrops. These complications are extremely rare, and in some babies a borderline or slightly increased nuchal fold can look normal on a repeat scan, especially if the first measurement was technically difficult.
No, they are not the same. They are only similar in that both are found at the back of the baby’s neck.
Increased nuchal fold (NF) is a thickening of the skin and tissue at the back of the neck, usually measured around 18–21 weeks as a soft marker.
Cystic hygroma is a large fluid-filled space or sacs at the back of the neck, often seen earlier in pregnancy and more strongly associated with chromosomal or genetic conditions and lymphatic problems.
They look different on ultrasound, have different causes and risks, and are managed in different ways. If a cystic hygroma is suspected, you should be referred to a fetal medicine specialist for detailed assessment and counselling.
For medical professionals who want to learn more about the SMART NT approach, access training, and join our clinical network.