SMART NT is a comprehensive, state-of-the-art approach to increased NT at 10 weeks, combining advanced ultrasound and KNOVA NIPT to support earlier and more precise assessment.

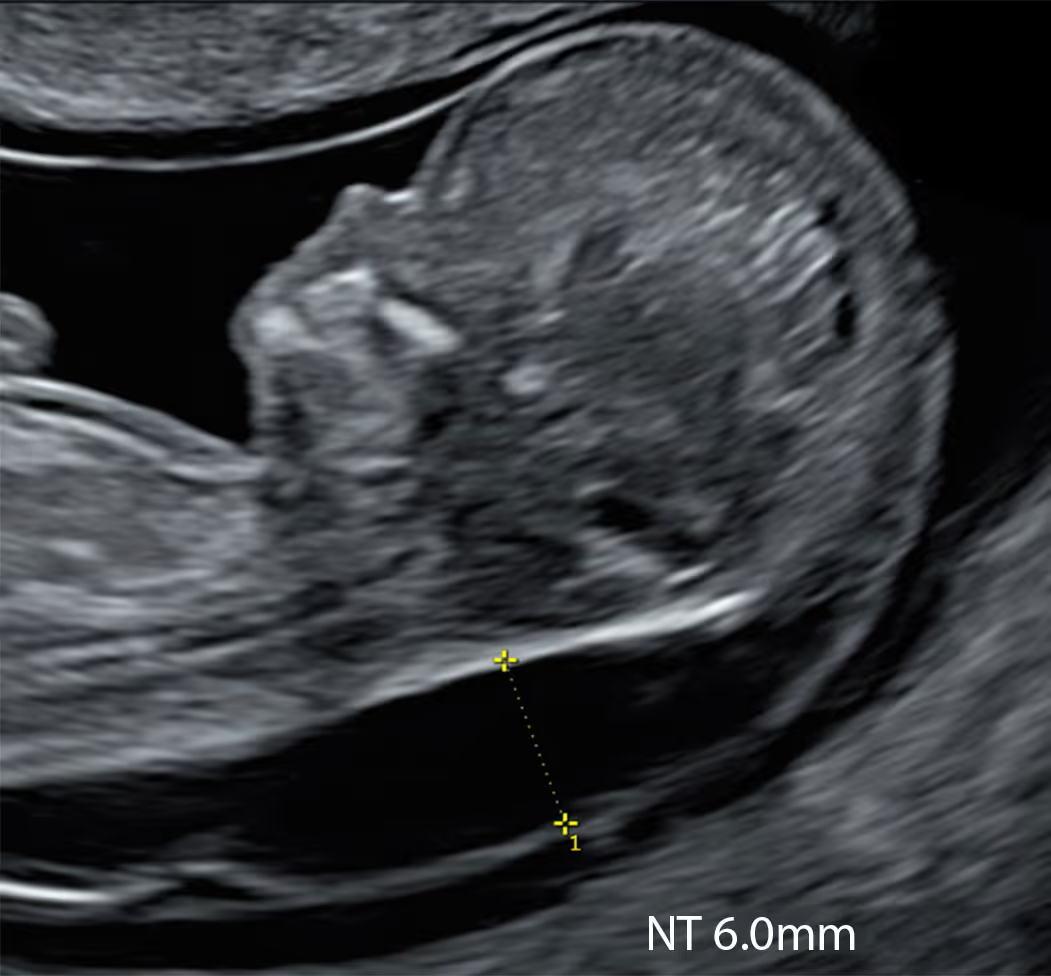
Nuchal translucency (NT) is the most powerful early indicator of a baby’s health.
Even when the NT improves, there is still about a 20% chance of an underlying condition.
Many people wrongly think that increased NT is linked only to Down syndrome.
SMART NT covers NT-related conditions in three categories: structural, chromosomal and genetic.
The SMART Test® is an advanced, one-stop screening performed at 10 weeks of pregnancy. It combines the earliest detailed anomaly scan using state-of-the-art ultrasound with the most advanced non-invasive genetic blood test (NIPT). SMART Test® is a registered trademark owned by London Pregnancy Clinic (LPC).
SMART NT is a specialised, two-step version of the SMART Test® designed for babies with increased NT. It also includes a targeted follow-up scan at 12–13 weeks to assess for structural anomalies linked to increased NT, such as serious heart defects.
This pathway is designed for pregnancies where an early increased NT has been identified. The SMART NT includes two detailed ultrasound scans — at 10 weeks and 12–13 weeks — together with an advanced non-invasive prenatal test (NIPT).
SMART NT applies at 10+0 to 11+1 weeks, when the CRL is 30.0–44.9 mm. It is not applicable to the standard NT assessment window used for the Combined Screening Test at 11–14 weeks, when the CRL is 45–84 mm.
“SMART NT” is available for general use; however, it should only be used to describe pathways that meet the criteria developed by Dr Fred Ushakov.
Our new approach to early prenatal diagnostics.
1
If increased NT is found, you can have the SMART Test straight away
2
Receive genetic results in 2 weeks
3
Top-to-toe expert fetal examination
Disclaimer! These reflections are my own and arise from practice rather than committee. They do not represent the positions of the FMF, UCLH, NHS, RCOG, ISUOG, or any other organisation. As with any clinician, I may make mistakes or misjudgements. In my view, a carefully performed 10 Week Scan, used alongside appropriately selected modern NIPT and followed by targeted diagnostic testing when indicated, can provide a balanced clinical approach by supporting earlier risk assessment while avoiding unnecessary intervention or over-interpretation. Dr Fred Ushakov
The SMART NT offers three key advantages over the traditional approach:
Early: Performed at 10 weeks rather than 12, providing the earliest possible insight into your baby’s health.
Comprehensive: Screens for a wide range of genetic syndromes and structural anomalies, especially heart defects, rather than focusing only on Down syndrome.
Non-invasive: Completely safe for both mother and baby, with no risk to the pregnancy.
By the time most parents are having their routine 12-week scan, the SMART Test® NT already provides both genetic and structural information about the baby with increased NT, offering valuable early reassurance or guidance.
Please note: SMART NT is a screening test, not a diagnostic one. It cannot exclude all possible conditions, and any high-probability results should be confirmed by diagnostic testing.
No. Invasive diagnostic tests such as chorionic villus sampling (CVS) cannot be safely performed at 10 weeks. At this very early stage, the baby’s limbs are still forming, and inserting a needle or sampling instrument through the womb can sometimes interfere with their development. This may sometimes result in transverse limb defects - where part of an arm or leg, especially a hand or foot, is absent.
For this reason, CVS is only recommended from about 11 weeks of pregnancy, when the risk of such complications is no longer present. At 10 weeks, only non-invasive options such as advanced ultrasound and NIPT can be used safely.
If a fetus shows increased NT at 10 weeks, the usual approach in many healthcare systems (for example, in the UK’s NHS) is to wait for the routine first-trimester scan and Combined Screening Test (CST) at around 12 weeks. By that time, approximately 50% of babies will show improvement, with NT measuring below the 3.5 mm cut-off used in standard screening programmes. However, even in this group, around 20% may still have an underlying condition and can receive a high-chance CST result.
For fetuses with persistently increased NT and/or a high-chance CST result, diagnostic options such as CVS or amniocentesis become available, alternatively a basic NIPT may be offered that screens only for trisomies 21, 18, and 13. In some countries, private NIPT can be performed earlier, from 10 weeks, but standard NIPT screens only for common chromosomal conditions and misses many genetic syndromes and structural anomalies linked to increased NT.
Both of these traditional pathways - waiting for combined screening or performing standard NIPT - often lead to delayed and incomplete diagnosis. The SMART NT protocol was created to address these limitations, providing an earlier, safer, and more comprehensive assessment for families worldwide.
No. There are some technological limitations with current genetic testing methods.
While the SMART NT works well for most singleton pregnancies, including those conceived through IVF, it is not suitable for multiple pregnancies (twins or triplets), donor egg pregnancies, or cases of vanishing twin syndrome.
There are also certain maternal contraindications, such as malignancy, a history of bone marrow or organ transplantation, and a few other rare medical conditions.
The SMART Test® was developed and introduced in the early 2020s by Dr Fred Ushakov, Director of the London Pregnancy Clinic (LPC), London, UK.
SMART NT is a modified version of the SMART Test® pathway, specifically tailored for fetuses with increased NT identified at the 10 Week Scan.
SMART Test® is a registered trademark of LPC.
The term “SMART NT” may be used freely, but it should only be applied when the pathway meets the criteria defined by Dr Fred Ushakov.
Disclaimer! These reflections are my own and arise from practice rather than committee. They do not represent the positions of the FMF, UCLH, NHS, RCOG, ISUOG, or any other organisation. As with any clinician, I may make mistakes or misjudgements. But I believe that coupling a careful 10 Week Scan with modern NIPT, and escalating to targeted diagnostics when indicated, offers families the balance we seek: early clarity without haste, and precision without noise.
Conditions associated with high Nuchal Transluncency (NT)
SMART NT is a structured pathway we use when the baby’s nuchal translucency (NT) is measured at around 10 weeks and is found to be increased. It combines a highly detailed 10 Week Scan, advanced blood tests (KNOVA NIPT) and follow-up scans to look early and safely for the main chromosomal, genetic and structural causes of increased NT.
Increased NT means there is more fluid than expected at the back of the baby’s neck for that gestational age. At 10 weeks this can be an early sign of chromosomal conditions (such as Down syndrome), certain genetic syndromes, heart defects or other structural problems; but it can also be a temporary or benign finding. SMART NT is designed to sort these possibilities out step by step.
Sometimes, because of the baby’s position, the tilt of the uterus, your build, or simply because at 10 weeks the fluid layer is extremely thin, the NT cannot be measured reliably. In this situation we still look very carefully at the neck region and save images. If we do not see a clear pocket of increased fluid, this is reassuring specifically in relation to increased NT, and from our extensive experience a truly increased NT at 10 weeks is usually very obvious.
If the reason we cannot measure NT is that the fluid layer is simply too small to see, that is generally good news. However, this does not replace other screening: we will usually recommend at least basic NIPT and an early anomaly scan, and a repeat scan around 12 weeks (either with us or with your usual antenatal care provider, such as the NHS in the UK).
SMART NT is usually reserved for cases where the NT at around 10 weeks can be clearly measured and is found to be increased (more than 95th centile).
In most services NT is measured at 11–14 weeks. In SMART NT, we bring this forward to about 10 weeks, using high-resolution ultrasound. This allows us to spot increased NT earlier, start investigations sooner and, if needed, give you answers and options earlier in pregnancy.
A normal NT at 10 weeks is reassuring for that specific marker, but it does not rule out most fetal anomalies or genetic syndromes. In fact the majority of affected babies actually have a normal NT. The SMART NT pathway is reserved for pregnancies with increased NT at 10 weeks, so if your baby’s NT is clearly normal you would not usually enter the SMART NT protocol.
However, we would still strongly recommend:
- At least a basic NIPT for Down’s syndrome (trisomy 21), and usually also trisomies 18 and 13.
- Early anomaly scans with a fetal medicine specialist (for example at around 12–13 weeks and again later in the second trimester) to look in detail at the baby’s structure.
- For parents who want broader information, we may also discuss an extended NIPT panel such as KNOVA, which can screen for additional chromosomal and selected genetic conditions not associated with increased NT.
So, while you are not in the “increased NT” group, careful screening with NIPT and early anomaly scans is still very important.
SMART NT is a clinical care pathway, not a research trial. It has been developed from many years of experience in fetal medicine, drawing on robust evidence from published studies together with modern advances in ultrasound and genomic testing.
Parents are not “recruited”, randomised or exposed to experimental procedures. Instead, SMART NT organises already validated high-resolution ultrasound and modern genomic tests into a structured, early pathway for pregnancies with increased NT.
Fetal anatomical scans at 10–14 weeks have been validated in multiple large studies around the world, including hundreds of thousands of fetuses. The ability to detect heart anomalies in the first trimester has been confirmed by a major meta-analysis of more than 300,000 fetuses.
Likewise, genomic technology for monogenic NIPT has been validated in multiple research studies, and in some countries (including NHS England) this technology is even used in a diagnostic context under the term NIPD (non-invasive prenatal diagnosis), rather than purely as screening NIPT.
So, while data from SMART NT is strictly audited, for you as a parent it is offered as up-to-date, evidence-based routine clinical care – not as participation in an experimental study.
For medical professionals who want to learn more about the SMART NT approach, access training, and join our clinical network.

Lorem ipsum dolor sit amet conse ctetur adip iscing elit justo quis odio sit sit ac port titor sit males dolor sit consectur dolor.

Lorem ipsum dolor sit amet conse ctetur adip iscing elit justo quis odio sit sit ac port titor sit males dolor sit consectur dolor.

Lorem ipsum dolor sit amet conse ctetur adip iscing elit justo quis odio sit sit ac port titor sit males dolor sit consectur dolor.

Lorem ipsum dolor sit amet conse ctetur adip iscing elit justo quis odio sit sit ac port titor sit males dolor sit consectur dolor.

Lorem ipsum dolor sit amet conse ctetur adip iscing elit justo quis odio sit sit ac port titor sit males dolor sit consectur dolor.

Lorem ipsum dolor sit amet conse ctetur adip iscing elit justo quis odio sit sit ac port titor sit males dolor sit consectur dolor.